A ‘Smart’ Insulin Patch May Aid Future Therapies

A smart insulin patch, once translated for humans, could eliminate the need for constant blood testing and help diabetics maintain a more consistent level of blood glucose.
Yanqi Ye, a Ph.D. student in biomedical engineering, was home in China last year when her NC State professor, Zhen Gu, asked if she could present a paper at a conference there. It became an “ahha” moment for Ye, helping her to see what a difference her research project could have in the lives of diabetics.
Ye talked about the research she has been working on in biomedical engineering: using a smart insulin patch to detect glucose levels and administer insulin in mice. Once translated for humans, it could eliminate the need for constant blood testing and help diabetics maintain a more consistent level of blood glucose. Though the project is still in animal trials, the idea impressed one man at the conference so much that he invited his diabetic father to come to the conference to meet Ye.
“His dad has very serious diabetes—late stage diabetes. He suffered a lot from leg pain, one of the diabetic complications. His doctor forced him to inject the insulin, but he didn’t like that,” Ye said.
The man’s father wanted to know when the smart insulin patch might be ready for human use. Though human trials are still years away, meeting a person who would actually benefit from her research inspired Ye.
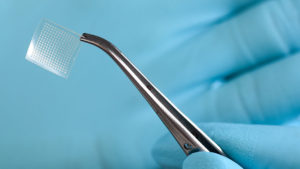
The smart insulin patch that Ye is studying in mice combines the nanotechnology of tiny pyramid-shaped microneedles with pancreatic cells that detect glucose levels. The needles in the patch—each 800 micrometers long and thinner than a human hair—penetrate only the top layer of skin, making it painless. She carries a sample of the mouse patch in a petri dish; it is about the size of a fingernail, with an array of needles, in rows 11 x 11.
A patch for human use would be larger—with 30 x 30 rows of needles that could be conical or pyramid-shaped. The pancreatic cells in the patch detect a person’s glucose levels, then administer insulin through the skin if required.
“In a healthy body, pancreatic cells regulate the hormone insulin. Diabetics can’t produce enough insulin, so they have high glucose levels because of low insulin,” Ye said.
Other technologies, like insulin pumps, require diabetics to monitor their own blood sugar levels. “It’s hard to control the accurate insulin injection,” Ye said. “A higher or lower dose can cause complications, like seizures, brain damage or death. If insulin gets too low, it can cause blindness or kidney failure.”
There is also a therapy for diabetics that involves transplanting pancreatic cells into the body to help regulate insulin, but the procedure is expensive and invasive for the patient. The patch allows for the same type of therapy—using pancreatic cells to regulate insulin—but the pancreatic cells remain outside the body in the smart patch.
Ye came to NC State originally as an undergraduate in a College of Textiles’ exchange program. Even then, she had an interest in biomedical fibers and medical devices. She had always wanted to visit the United States, urged on by her father, a businessman, who had traveled here.
While finishing her undergraduate degree, she learned about the biomedical engineering program, a joint program between NC State and the University of North Carolina at Chapel Hill. Students in the program attend classes at both universities—there is even a shuttle that transports students between the two campuses in Raleigh and Chapel Hill, about 30 miles apart.
The program combines the strengths of NC State’s College of Engineering with the human medicine programs at UNC. The resources from both campuses contribute to the strength of the biomedical engineering programs, Ye said.
When Ye first approached Gu about joining his lab in 2013, the program consisted of four graduate students and two postdocs. “I showed him what I had been doing in textiles, then I volunteered in his lab for a semester. He thought I was ready (for graduate school),” she said.
Today, Gu’s lab staff and research program have grown, supporting six graduate students and five postdocs, Ye said. Though she’s been with the lab for about four years, Ye calls herself, “the grandmother” in the graduate program.
In fact, the research has been so successful, that Gu has cofounded a Research Triangle Park company Zenomics Inc. aimed at commercializing the technology and making it available around the world. Zenomics has received substantial investments from the Chinese company MicroPort Scientific.
Ye’s achievements in graduate school extend beyond the lab. In December 2016, the Analytical Instrumentation Facility chose her paper, “Microneedles Integrated with Pancreatic Cells and Synthetic Glucose-Signal Amplifiers for Smart Insulin Delivery,” as one of two “best papers” for 2016. The paper was originally published in Advanced Materials.
A year ago, she was one of five NC State graduate students to receive conference awards from the Graduate Student Association. Ye attended the 2016 AlChE Annual Meeting in San Francisco. She also earned an honorable mention for a research image she submitted to a scientific art competition of the Research Triangle Nanotechnology Network, a partnership between NC State, Duke University and UNC-Chapel Hill.
I really want to see one day that we can work with an industrial company to put this into the market for the patient to actually use it.
In addition to the smart insulin patch, Ye is working on a cancer immunotherapy patch using melanin against melanoma, a skin tumor that is usually cancerous. The vaccination patch was applied to the skin of healthy mice. Even after tumor cells were introduced to the vaccinated mice, all the test mice survived for at least two months, and 87 percent did not develop any tumors. This work has been accepted for publication by the journal Science Immunology.
The patch could also be used to deliver immunotherapeutic drugs directly to the skin tumor, through microscopic needles that are conical-shaped, a therapy that appears to be effective in mice, Ye said.
The cancer research is personal for Ye. Before she left China to come to NC State as an undergraduate, her grandmother was hospitalized, and later died from late-stage metastatic cancer.
“She suffered a lot,” Ye said. “It ignited my passion to study biomedical engineering.”
Ye’s mother, a high school teacher in China, always wanted Ye to become a doctor. Ye believes that her biomedical engineering is fulfilling her mother’s desire for her to work in medicine—and she’s proud of where her research is heading.
Clinical trials in humans for both of these technologies are still years away, Ye acknowledges. But meeting the diabetic man in China has strengthened her commitment to her research.
“Of course, I hope to see the translation of this technology (to human medicine),” Ye said. “The most impressive memory for me is definitely the conversation between me and that diabetic patient. It really ignited my passion for translating that technology to really benefit the patient.
“Right now, we’re just doing the research in the lab, and we don’t have a chance to communicate with the patient,” Ye said. “I really want to see one day that we can work with an industrial company to put this into the market for the patient to actually use it.”
“One day” for Yanqi Ye could mean continuing her research as a postdoc or in an industrial lab to translate the technology for human medicine. And one day, maybe she will meet a patient whose life is changed through her research efforts.
DIABETES ON THE RISE
The number of people with diabetes has nearly quadrupled since 1980. Prevalence is increasing worldwide, particularly in low- and middle-income countries. The causes are complex, but the rise is due in part to increases in the number of people who are overweight, including an increase in obesity, and in a widespread lack of physical activity.
Diabetes of all types can lead to complications in many parts of the body and increase the risk of dying prematurely. In 2012 diabetes was the direct cause of 1.5 million deaths globally. A large proportion of diabetes and its complications can be prevented by a healthy diet, regular physical activity, maintaining a normal body weight and avoiding tobacco use.
FOR FURTHER READING:
Skin Patch Dissolves Fat; Could Help Treat Diabetes
Scientists Create Painless Patch of Insulin-producing Beta Cells to Control Diabetes
Microneedle Patch Delivers Localized Cancer Immunotherapy to Melanoma
Download this article as a PDF.
- Categories:


